Table of Contents
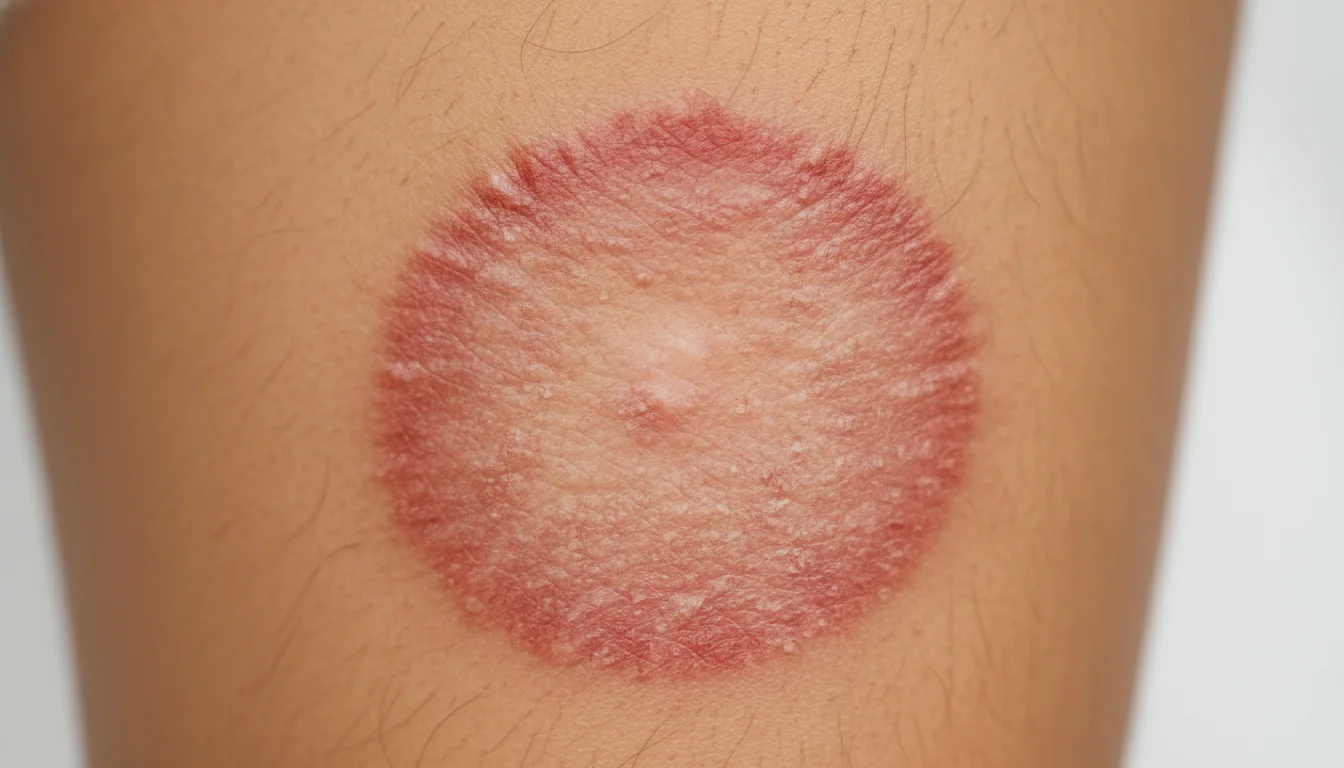
Knowing how to get rid of jock itch sounds simple – buy a cream, apply it, done. Except it keeps coming back for most people. Jock itch (tinea cruris) is a fungal infection of the groin, upper thighs, and buttocks. The same fungus that causes athlete’s foot and ringworm. It’s not dangerous, but it doesn’t go away on its own – and half-treating it is why most people end up dealing with it for months. The rash looks better, you stop treatment, it comes back. Here’s how to actually end it.
1. Apply Topical Antifungal Cream
This is the treatment. Everything else on this list supports it.
OTC antifungal creams are the first-line fix: terbinafine (Lamisil AT), clotrimazole (Lotrimin AF), or miconazole (Micatin). Terbinafine is the one to reach for if you want it gone faster. It’s fungicidal, meaning it kills the fungus rather than just stopping it from reproducing. Clotrimazole and miconazole are fungistatic – they inhibit growth and rely on your immune system to finish the job. That takes longer: two to four weeks versus one to two for terbinafine.
How to apply it:
Apply twice daily. Clean thin layer, not a thick glob – thick application wastes product and doesn’t improve penetration. The important part most people miss: extend the cream 1 inch (2.5 cm) beyond the visible rash edge. The fungus has already spread past where the inflammation appears, so stopping at the visible border leaves live cells to regrow. That’s the margin where recurrence starts.
Don’t cover the area with an occlusive bandage after applying. Covering it traps moisture, which is exactly what dermatophytes need to persist.
Keep going after it looks gone. This is where most people fail. Stopping when the rash looks better leaves residual fungal cells in the skin margin – they’re still there, just not inflamed enough to be visible. Continue for at least one full week after you can’t see the rash anymore. Under-treatment is the single most common reason jock itch comes back, often within a week or two of stopping.
Course lengths by product:
- Terbinafine: 1-2 weeks for tinea cruris
- Clotrimazole or miconazole: 2-4 weeks
If there’s no visible improvement after two weeks of consistent twice-daily use, stop guessing. Either the diagnosis is wrong (seborrheic dermatitis and psoriasis look identical to jock itch) or you need prescription-strength treatment. A dermatologist can confirm with a scraping in the office. Prescription econazole or clotrimazole at higher concentrations work where OTC fails in some cases.
2. Wash the Area Before Applying Cream
Soap and water before the cream isn’t optional – it’s what makes the cream work properly.
Fungal cells, sweat residue, sebum, and dead skin on the surface physically block topical treatments from contacting the skin layer where the infection is established. The sequence matters: wash, dry thoroughly, apply cream. Applying cream to an unwashed or still-moist surface reduces how well it penetrates.
Technique:
Use lukewarm water, not hot. Hot water increases skin irritation and can worsen inflamed skin. Apply a small amount of mild soap and lather gently with your fingertips – not a rough cloth while the skin is active and irritated. Rinse completely. Soap residue left on skin causes contact irritation. Pat dry immediately and thoroughly.
On soap choice: Antibacterial soap won’t kill fungal infections (antibacterial and antifungal work on completely different biological targets), but it does reduce secondary bacterial load that can complicate presentation. Fragrance-free, mild soap is better if the skin is visibly inflamed. Skip anything with heavy moisturizers or emollients in the affected area – they increase moisture retention.
Once daily is enough. More frequent washing strips the skin barrier and makes the irritation worse, not better.
3. Keep the Skin Dry After Bathing
Moisture is the condition jock itch needs to persist. You can apply cream correctly and still drag out the infection by getting dressed while the skin is still damp.
Pat dry with a clean towel – don’t rub. Rubbing spreads fungal cells to adjacent skin and abrades already-irritated tissue. Work explicitly through the skin folds in the groin: these areas retain moisture long after the surrounding skin is dry because the skin surfaces press against each other. After patting, let the area air dry for one to two minutes before putting clothes on. That brief window removes residual moisture that patting alone won’t fully get.
Use a clean, dry towel each time. A damp towel reintroduces moisture and may harbor fungal cells from a previous use. During an active infection, wash towels and underwear in hot water after each use – fungi survive on fabric and can reinfect cleaned skin.
This isn’t a cure. It’s a habit that removes the environmental conditions the infection needs between cream applications.
A note on laundry that most guides skip: wash the clothes and towels that contact the affected area in hot water (at least 140°F / 60°C) throughout the treatment period. Fungal spores survive a cold-water wash. Reusing contaminated towels or underwear between washings can reintroduce fungal material to skin you’ve just cleaned. Hot wash, fresh towel each use – it’s a small thing that makes a real difference over a two to four week treatment course.
4. Apply Absorbent Powder Between Applications
Antifungal cream twice a day leaves several hours in between where moisture builds back up. Absorbent powder fills that gap.
Corn starch works. Talc-free baby powder works. If you want the powder to do antifungal work as well, Zeasorb-AF contains miconazole and handles both moisture absorption and direct fungal suppression.
How to apply it: Apply a light, even dusting to bone-dry skin – after you’ve patted and air-dried, before putting clothes on. Light coating, not a thick layer. Too much powder cakes up and traps moisture instead of absorbing it. The goal is a thin film that wicks sweat as it forms.
This is supporting cast, not the main treatment. It doesn’t replace antifungal cream. It creates worse conditions for the fungus between your twice-daily applications.
5. Wear Loose, Breathable Fabric
Tight synthetic underwear turns the groin into a warm, humid environment. That’s exactly what the fungus needs.
Cotton or moisture-wicking athletic fabric that actually breathes (not just marketed as "performance") keeps the area drier throughout the day. Loose fit matters more than the specific fabric. A loose-fitting cotton boxer does more work here than tight-fit compression shorts, even if the shorts claim to wick moisture.
If you’re prone to recurring jock itch, clothing choice is how you prevent it from coming back after you’ve cleared it. Synthetics aren’t the enemy in general – they’re the enemy for this specific application.
6. Oral Antifungal Medication (When Cream Isn’t Enough)
Topical cream fails sometimes. If you’ve been consistent – twice daily, beyond the rash edge, for a full four weeks – and the infection is still there or keeps coming back, you need to see a doctor.
At that point there are two possibilities: the diagnosis is wrong (a skin scraping and culture will confirm in minutes), or the infection is established deep enough that topical cream can’t reach it effectively. Oral medication treats this systemically.
What gets prescribed:
Oral terbinafine (Lamisil) is the standard prescription for dermatophyte infections. The typical course is two weeks at 250 mg daily. Cure rates above 90%. It’s fungicidal, same mechanism as the cream but delivered through the bloodstream instead of the skin surface. It’s metabolized by the liver, so baseline liver function tests may be ordered for extended courses, and it shouldn’t be used by people with active liver disease.
Fluconazole (an azole antifungal) is sometimes prescribed as an alternative, particularly if terbinafine is contraindicated. It’s fungistatic rather than fungicidal, often given as a weekly dose for several weeks.
Before starting: confirm the diagnosis. Skin conditions that mimic jock itch don’t respond to antifungals, and taking a systemic medication for something that isn’t there carries real side effect risk for no benefit. Also check your medication list – azoles in particular interact with a wide range of drugs (they inhibit CYP3A4).
Don’t go in asking for oral antifungals on the first visit. Topical treatment works for most cases and carries zero systemic risk. Oral medication is the right tool when topical has genuinely failed.
Prevention
Once you’ve cleared it, keeping it gone is mostly about moisture management.
Dry thoroughly after every shower – air dry for a minute before dressing. Change into clean, dry underwear after exercise; don’t stay in workout clothes once you’ve stopped moving. Apply absorbent powder as a daily habit if you sweat heavily in that area. Treat athlete’s foot aggressively if you have it – the same fungus spreads from feet to groin via towels and hands. Use sandals in communal locker rooms and pool changing areas.
If you’re getting recurring jock itch despite treating it fully each time, ask whether you’re reinfecting from a source: contaminated towels, a partner with an untreated fungal infection, or persistent athlete’s foot that keeps seeding the groin.
When to See a Doctor
Four weeks of consistent OTC treatment with no improvement is the main signal. At that point, confirm the diagnosis before trying anything else. Seborrheic dermatitis, psoriasis, erythrasma (bacterial, not fungal), and contact dermatitis all look identical to jock itch and don’t respond to antifungals. A dermatologist can do a KOH scraping in the office and give you a confirmed diagnosis.
Also see a doctor if the rash is spreading rapidly, developing blisters or pustules, or if you have fever alongside it. That combination can indicate a secondary bacterial infection that needs antibiotics, not antifungals.
Frequently Asked Questions
What is the fastest way to cure jock itch?
Terbinafine cream (Lamisil AT) applied twice daily. It’s fungicidal rather than fungistatic, typically clearing tinea cruris in one to two weeks. Apply it 1 inch (2.5 cm) beyond the visible rash edge and continue for at least one week after the rash disappears. That continuation step is what prevents recurrence.
Is jock itch a form of STD?
No. Jock itch is caused by a dermatophyte fungus in the same family as athlete’s foot and ringworm. It’s not sexually transmitted. It spreads via direct skin-to-skin contact, contaminated towels, and clothing. The groin location has nothing to do with sexual transmission.
What could be mistaken for jock itch?
Several things: seborrheic dermatitis, psoriasis, contact dermatitis (allergic reaction to fabric or soap), and erythrasma (a bacterial infection that creates a similar-looking rash in skin folds). The tell is treatment response – if OTC antifungal cream isn’t working after four weeks of consistent use, get a proper diagnosis before continuing treatment.
What triggers jock itch?
Warmth and sustained moisture in the groin. Heavy sweating, tight synthetic clothing, skin folds that trap humidity, and obesity (more skin overlap, more trapped moisture) are the primary factors. Having athlete’s foot is a major trigger most people don’t connect – the same fungus spreads from feet to groin on towels and hands. Communal changing rooms are also a common transmission source.